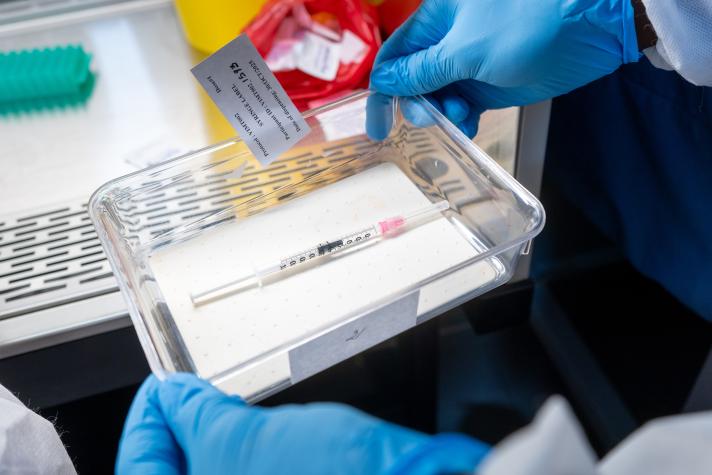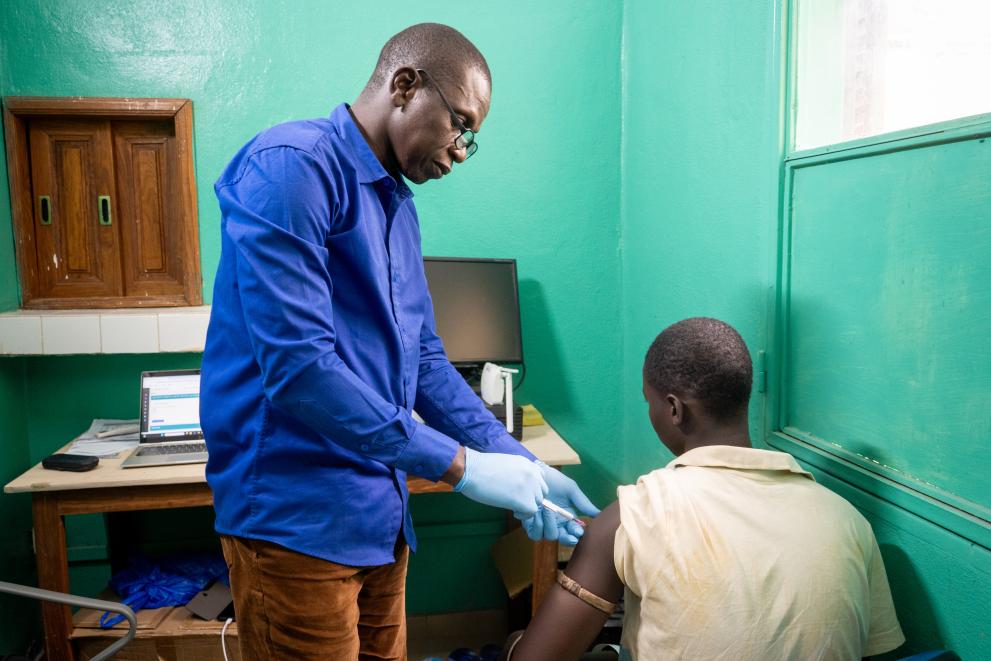
Over the past 50 years, the sustained use of vaccines has contributed to saving more than 150 million lives, equivalent to around six lives every minute. Despite this progress, there are still significant gaps in vaccine coverage. In 2024, an estimated 20 million children missed essential routine vaccinations, including more than 14 million zero-dose children who received no vaccines, according to the World Health Organization.
These gaps are driven by persistent inequities in the reach and design of health systems. Many zero-dose children remain outside any formal healthcare structures due to living in remote or marginalised communities; vulnerable children often lack sustained protection during high-risk recovery periods, as existing interventions only cover a fraction of the time they remain at risk; and key populations, such as adolescent girls and pregnant women, continue to be underrepresented in clinical research and routine safety monitoring.
On World Immunization Week, these figures highlight the need for continued investment in vaccine research, development, and equitable deployment. In this context, Global Health EDCTP3, under the Horizon Europe programme, is currently funding 11 projects focused specifically on vaccines targeting malaria, childhood infectious diseases, and emerging and re-emerging infectious diseases, with a total investment of €63 million.
In this article, we highlight three ongoing Global Health EDCTP3-funded projects advancing immunisation through Europe-Africa partnerships.
REACH-OUT: closing the gap for zero-dose children
The REACH-OUT project focuses on developing equitable strategies to reach zero-dose children who are currently excluded from the benefits of immunisation programmes. These vulnerable infants often live in remote or marginalised communities and account for one-third of all childhood deaths in low- and middle-income countries. The project works alongside national immunisation programmes in Kenya, Nigeria, and Rwanda to identify the root causes of low vaccination rates by addressing both supply-side and demand-side barriers.
‘High vaccination coverage should always be considered as a historical achievement. All of us should be worried about those children missing vaccination and ensure no single child is left behind.’
Hassan Sibomana, EPI Director, Rwanda Biomedical Center
To improve targeting, the REACH-OUT team uses integrated geospatial and epidemiological models to create high-resolution maps of infection risks and service gaps. These data will provide a clearer picture of where zero-dose children are likely to live and generate evidence on the effectiveness of a range of interventions to improve access to and take-up of immunisation services.
R21-PD: protecting children following severe anaemia
The R21-PD project explores whether malaria vaccination can protect children who have been discharged from hospital after treatment for severe anaemia. Children in this category remain at an elevated risk of readmission and death for up to twelve months following their recovery.
While the World Health Organisation currently recommends post-discharge malaria chemoprevention, this strategy typically provides protection for only three to four months, leaving a significant period of vulnerability.
The project is conducting a clinical trial in moderate to high transmission areas of Kenya, Malawi, and Uganda to test whether an R21/Matrix-M malaria vaccine booster can offer longer-term protection. This theory suggests that a booster dose could generate a robust immune response during the critical post-discharge period while the child remains temporarily protected by standard antimalarial drugs.
PfVIMT: advancing next-generation malaria elimination
The PfVIMT project aims to move an innovative transmission-blocking malaria vaccine toward regulatory authorisation. While current vaccines primarily prevent the parasite from invading liver cells, there is a strategic need to target the gametocytes that mosquitoes ingest to infect others. This strategy reduces the total malaria burden in a community by breaking the cycle of transmission.
‘Current malaria vaccines are saving lives, especially among young children. But older children and adults still carry parasites and keep transmission going. Malaria parasites have a complex life cycle, and no single approach is enough. To move from control towards elimination, we need vaccines that reduce both disease and the transmission of parasites within communities.’
Nicaise Ndam, Project Coordinator, Institut de Recherche pour le Developpement, France
The project team is combining the existing R21/Matrix-M vaccine with a promising transmission-blocking candidate known as Pfs230D1. Following initial phase II studies in Mali, the safety and efficacy of this multi-stage vaccine will be confirmed in a multi-country phase III trial involving participants aged five and older.
A key feature of the research involves the use of direct skin-feeding assays to measure how effectively the vaccine prevents mosquitoes from picking up parasites from vaccinated individuals. This combination approach is designed to provide both individual protection and community-wide benefits, moving sub-Saharan Africa closer to the goal of malaria elimination.
Details
- Publication date
- 27 April 2026
- Author
- Global Health EDCTP3 Joint Undertaking